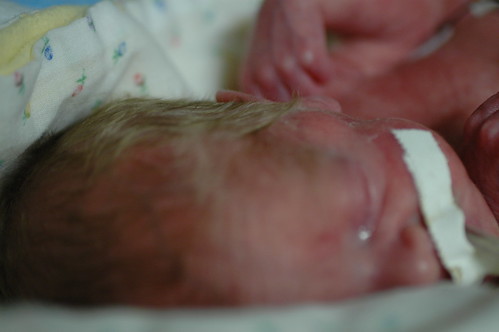
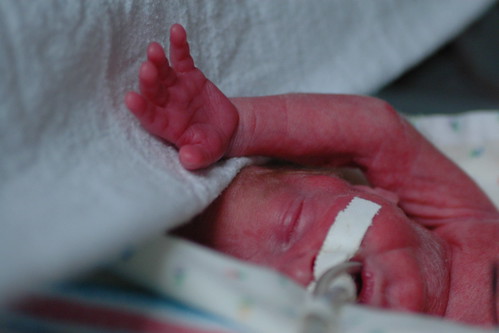
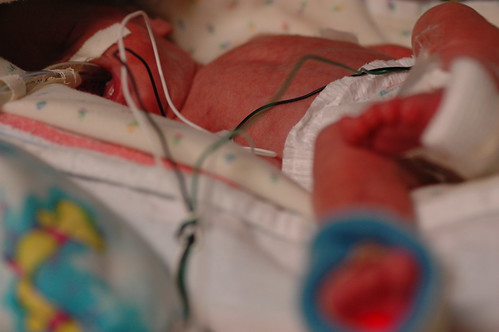
the good news is that eric’s overall clinical picture is improving, even though he is still on the vent, which is to say that his blood counts are showing that his systemic infection is nearly gone and his blood gas profile is looking great. the shortest answer as to why he’s on the vent for longer than he’s ever been is that they are concerned that they want to make sure that his bowels are completely recovered after shutting down the other day before they put him back on cpap. the armchair reseachers in the crowd can investigate why cpap is bad after an illeus ( the technical term for the lower bowels stopping to function ) because i haven’t had the time to put all the pieces together.
although his overall status is improving, we were warned about a few new issues that are developing. after 5 weeks of not needing much supplemental oxygen, eric is starting to need to have his ‘ooooooh’ increased; in other words, while he’s done remarkably well in the past breathing unenriched room air ( with around 20-21% oxygen) , he’s now consistently needing 25-40 percent oxygen in his air supply. of course, there are several reasons why he might be needing more oxygen.
most innocuously, he might simply be getting comfortable on the vent and getting lazy, taking fewer and shallower breaths. breathing takes a lot of work, and if the machine is going to do the heavy lifting, many micropreemies are more than happy to take a breather from breathing and require a little more oxygen to keep their blood gas levels at appropriate levels. while this might be partly the cause, he respiratory profile doesn’t indicate that he’s getting too lazy, so my guess is that it’s only playing a minor role.
slightly more disconcertingly, he may also be developing a tracheal infection, which can irritate his mucous membranes and produce more slime and goo than normal; more slime and goo makes it more difficult to breath and increase the need for supplemental oxygen. he certainly seems to have more secretions than normal of late. and indeed, while we were discussing the potential for trach bugs, eric’s latest labs came back and he was positive for enterobacter and klebsiella which are gram negative nosocomial bugs – in other words he got an infection from bugs that you find in the hospital. while it’s not something that you want to see, it would be more remarkable if he didn’t get a nosocomial infection from all the tubes entering various parts of his body. technically, the bugs have simply colonized and have not shown any evidence of becoming particularly invasive. simply put, they are just hanging out and slowly multiplying around his ET tube and don’t seem too concerned with overtaking his system. it’s very difficult to pummel colonized nosocomial bugs into complete submission so they are going to wait and see if eric’s nascent immune system can keep them in check. i guess you could call this a developing story that could “get legs” and hit the front page soon.
perhaps even more problematic is the fact that eric could be developing a lung condition known as chronic pulmonary insufficiency of prematurity (cpip). essentially, this means his lungs are not growing fast enough to keep up with the oxygen requirements demanded by his growing body. cpip presents itself similar to bronchopulmonary dysplasia (bpd), but they are actually different enough to warrant different treatment strategies. this evening nurse practitioner dawn was not willing to say that he definately had cpip, but she said it wouldn’t surprise her at all to see him get the official diagnosis over the coming weeks. the good news is that if he does have cpip, he will quite likely eventually regain normal lung function ( perhaps by year 2 ). the not-so-good news is that cpip could necessitate that he leave the nicu with an oxygen tank.
just in case you’ve started to miss the forest for the trees, the good news is that eric’s overall clinical picture is improving.
and we’re still getting postcards ( scroll down to the bottom of the link )!