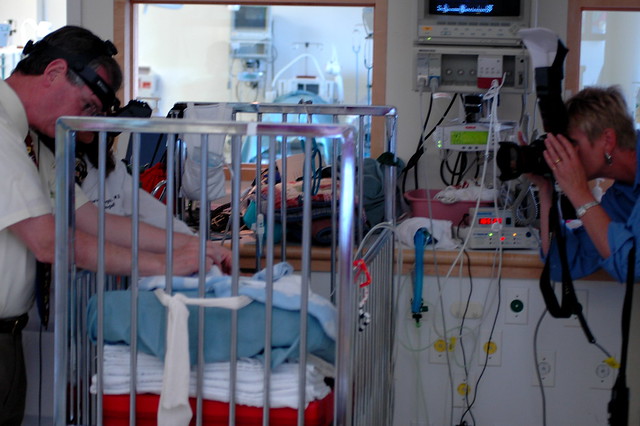
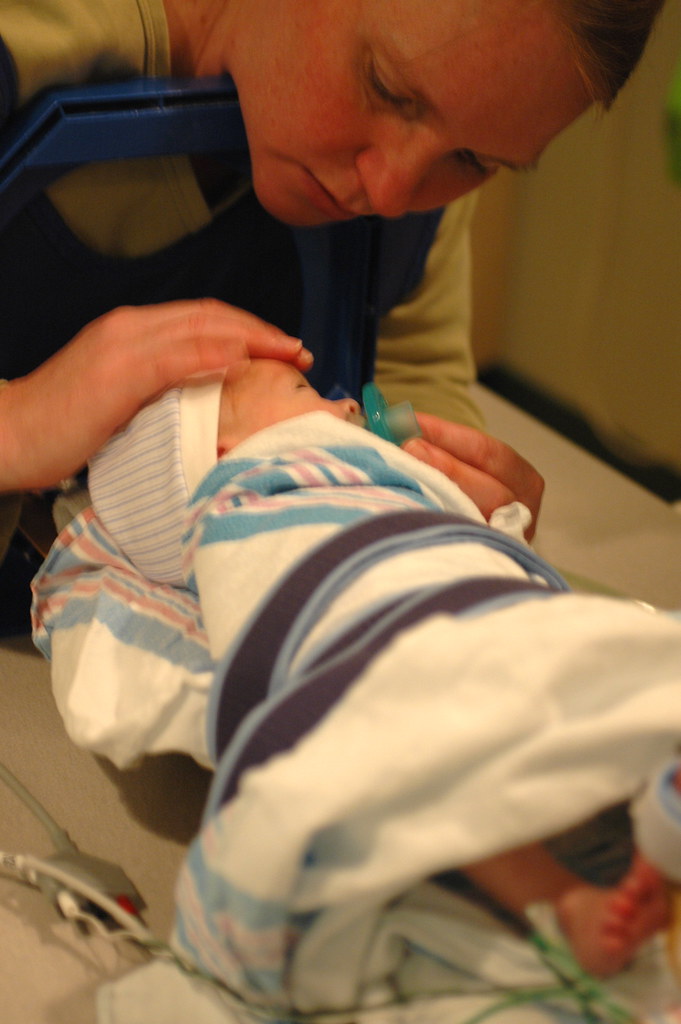
one of eric’s neonatologists from his old nicu stopped by today. she does research at the new nicu and after talking for a bit about how he was doing, she asked us if we’d allow her to have some pictures taken for a publication that they are putting together about the ROP research that she’s doing with eric’s opthamologist, dr. droste. of course, we were happy to have them take some pictures of little odin, on the condition that i could take a picture of them taking a picture of him.
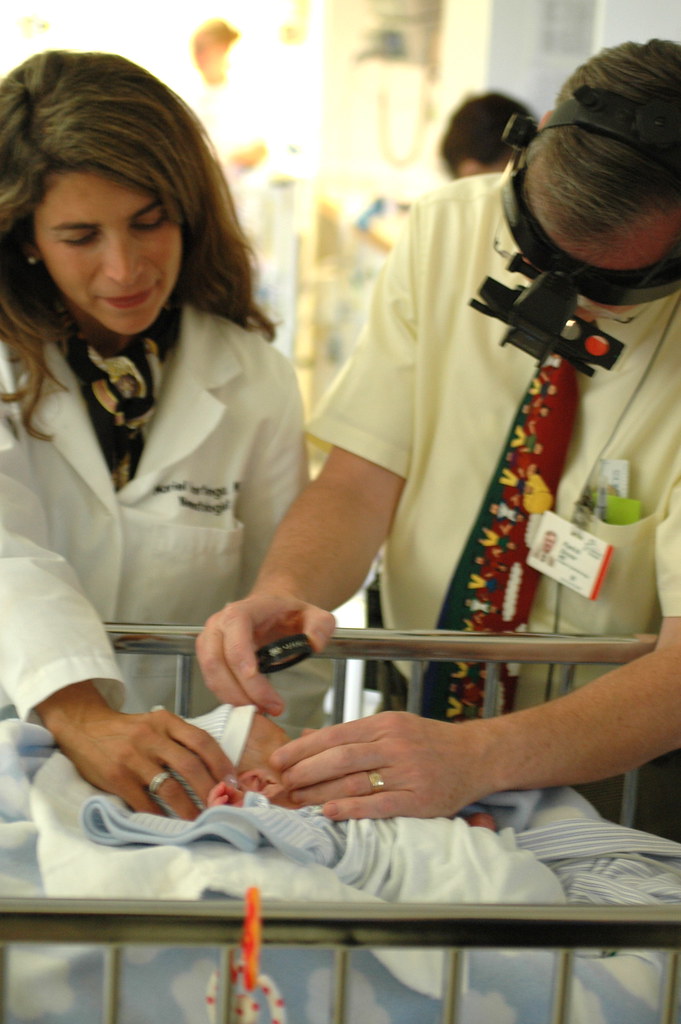
the man in the photos is dr. droste, who performed eric’s rop surgery and the woman in the lab coat is dr. poortenga. we like her a lot, since her quick actions helped to unstrangulate his strangulated hernia on day 35. had she not been successful eric would have been transferred to the new nicu much sooner for emergency surgery. she’s very nice and is one one of the many people that we were not able to get a picture with before leaving the old nicu, due to the quickness of the transfer – so it’s nice turn of events to finally get the picture afterall.
during the photo-op, dr. droste took a moment to perform a follow up exam for his recent rop surgery. the good doctor still thinks eric looks “good”, but believes he has a 50% chance of needing further surgeries ( which is a higher estimate that he provided immediately after the surgery). he also clarified that kids with disease similar to eric have a 20% chance of developing more severe ROP, an 80% chance of ending up with 20/100 vision or better and a 60% chance of having 20/50 eyesight or better. so, there’s a good chance that he’ll need some sort of eyeglasses in the future, but that was probably going to happen anyway, since nearsightedness runs in the family.
after the photo-op, we went on what eric’s nurse called a “field trip” for his upper GI exam. and what a field trip is was! i think i might have left the mistaken impression that we were overly concerned about the radioactivity of the barium during the exam. i guess it was poor wording on my part, since kris and i have both had upper GIs and know that while it’s not a risky exam, we know that it’s not exactly a walk in the park either and all things being equal we’d have preferred to not have to have him wheeled to a far corner of a hospital, strapped to a board and rotated around while drinking a barium milkshake. but that’s just us being worry wart parents, because eric simply couldn’t have cared less. he took it all in stride and, amazingly, didn’t cry once. he just looked around and calmly took it all in. i guess in the world of a micropreemie, it’s just another day in the nicu.
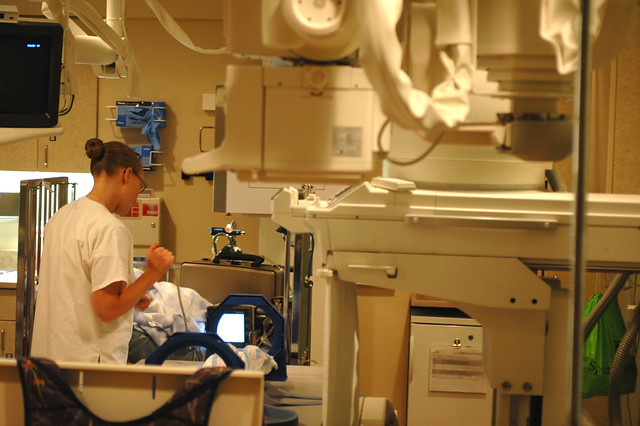
the exam room is small, but it’s filled with lots of equipment, including a large x-ray machine.
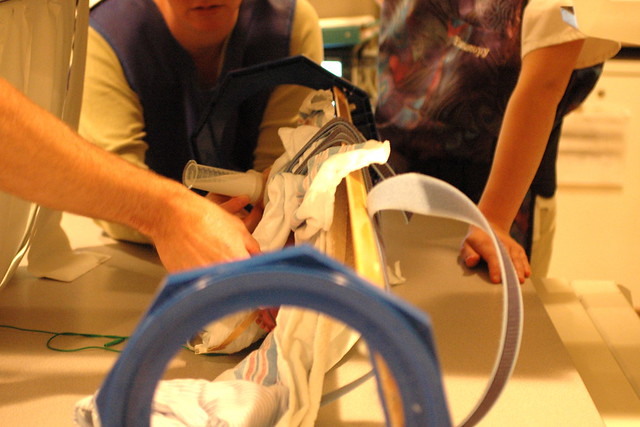
little odin is quickly place on a board that will allow the technical staff to rotate him 180 degrees to get a variety of views of the radioactive barium flowing through his digestive tract during the upper GI test.
eric is strapped to the board to prevent him from falling off during the procedure.
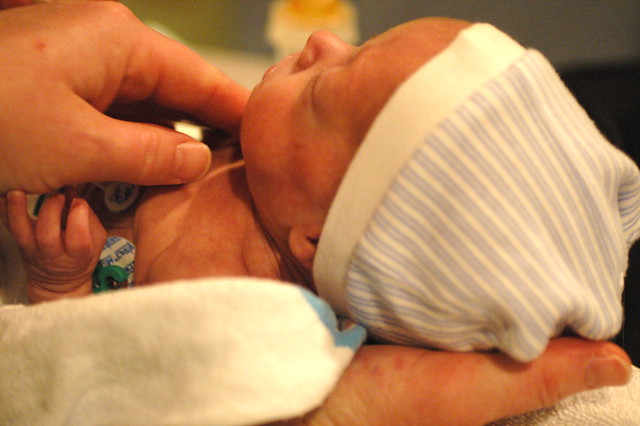
kris conforts eric right before the upper GI exam begins.
during the exam, they carefully rotate him while feeding him radioactive barium to get front and side views of his gastrointestinal tract while he’s feeding.
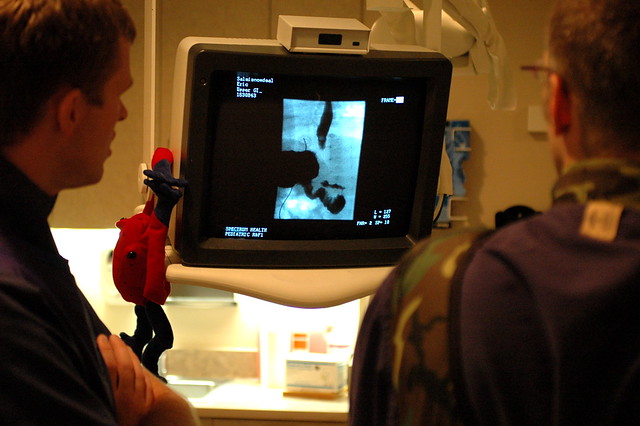
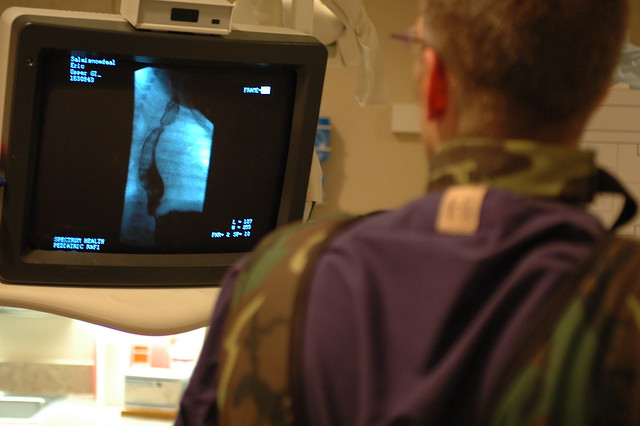
two techs, jeff and jeff, look at the x-ray movie as the food moves down his esophagus, into his stomach and enters his small intestine.
kris comforts eric after we believe the procedure is finished.
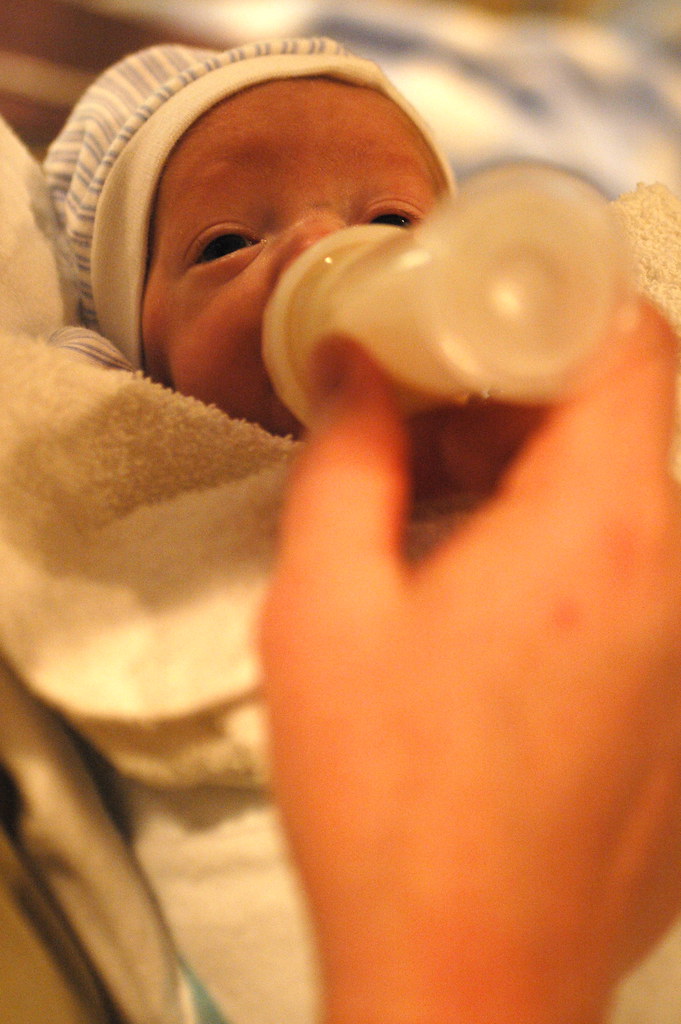
eric’s hungry, since they skipped his 12 a.m. feeding before the procedure, so kris gives him a bottle which he gulps down.
d’oh! right after kris gave eric his bottle we discover that they want to get a few more images to help them clarify an abnormality that they found in the initial test.
jeff looks on as he completes a second set of scans. he’s looking at the narrowing in eric’s esophagus, which – if you look carefully – you can see on the monitor. eventually he determines that the narrowing is simply a “tertiary contraction” which happens when his esophagus contracts in an uncoordinated manner that’s not uncommon in micropreemies and not – thankfully – a physical obstruction caused by abnormal vasculature.
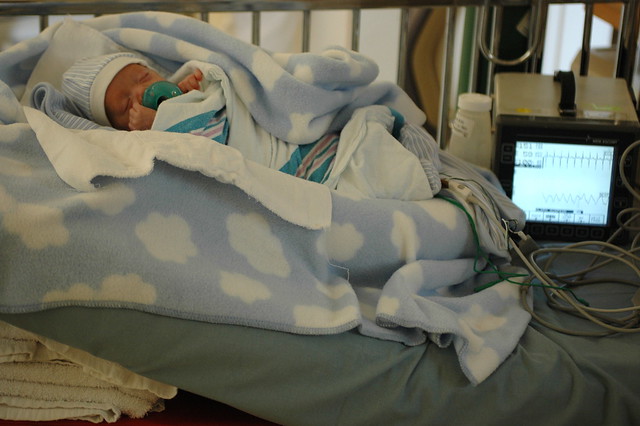
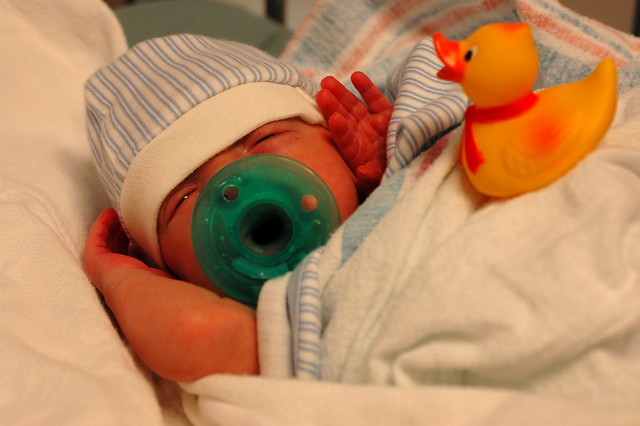
eric’s nurse gave him a “rubber ducky” for doing so well doing the procedure. after we return to the nicu, the duck looks on while eric sleeps since he’s very, very tired from such an exciting adventure.
unfortunately, they discovered that eric is refluxing almost as soon the milk hits his stomach, which is not good. the preliminary assessment is that he has an undiagnosed hiatal hernia, which happens when the stomach prolapses through the diaphragm. although it’s a relatively small hernia, it could still be the cause of why eric is refluxing so quickly. we don’t know much at this point and will have to wait until tommorrow when the pediatric surgeons get a chance to review the results of the upper GI. why would the pediatric surgeons be reviewing the upper GI? because the neonatologist’s hunch is that eric should have the hiatal hernia repaired and is also a candidate for a surgical procedure known as “nissen fundoplication” which strengthens the stomach valve. it’s hard to imagine that a little over a week ago, we were close to going home with eric and now it appears that we’ll need to make some quick decisions about an ever expanding list of surgical options.
while it seems reasonable to contemplate repairing the hiatal hernia, we were a bit surprised to hear that they also thought he might benefit from the nissen procedure, since my understanding is that it’s done as a last resort. perhaps they’d just like to do it if they already have to have him in the operating room. in any case, we’ll know more tomorrow after talking with the surgeons.
unfortunately, if he does need surgery, unlike the inguinal hernia surgery, they don’t often perform it on babies that weigh less than 2,500 grams, which means – under optimal conditions, we could be faced with another 10-20 days in the nicu, just waiting for him to gain enough weight for the surgery. and if he starts having problems gaining weight due to the reflux, then it could even longer.
temporarily abandoning the rollercoaster cliche’ in favor of the marathon metaphor – while things might look quite a bit different tomorrow after we talk with the pediatric surgeons, it’s hard not to feel like the finish line keeps moving farther and farther away.